- Precision Care for a Stronger Spine
- +91-8448479865
+91-8448479865
drprankulsneuro@gmail.com
ParkinsonÔÇÖs Surgery
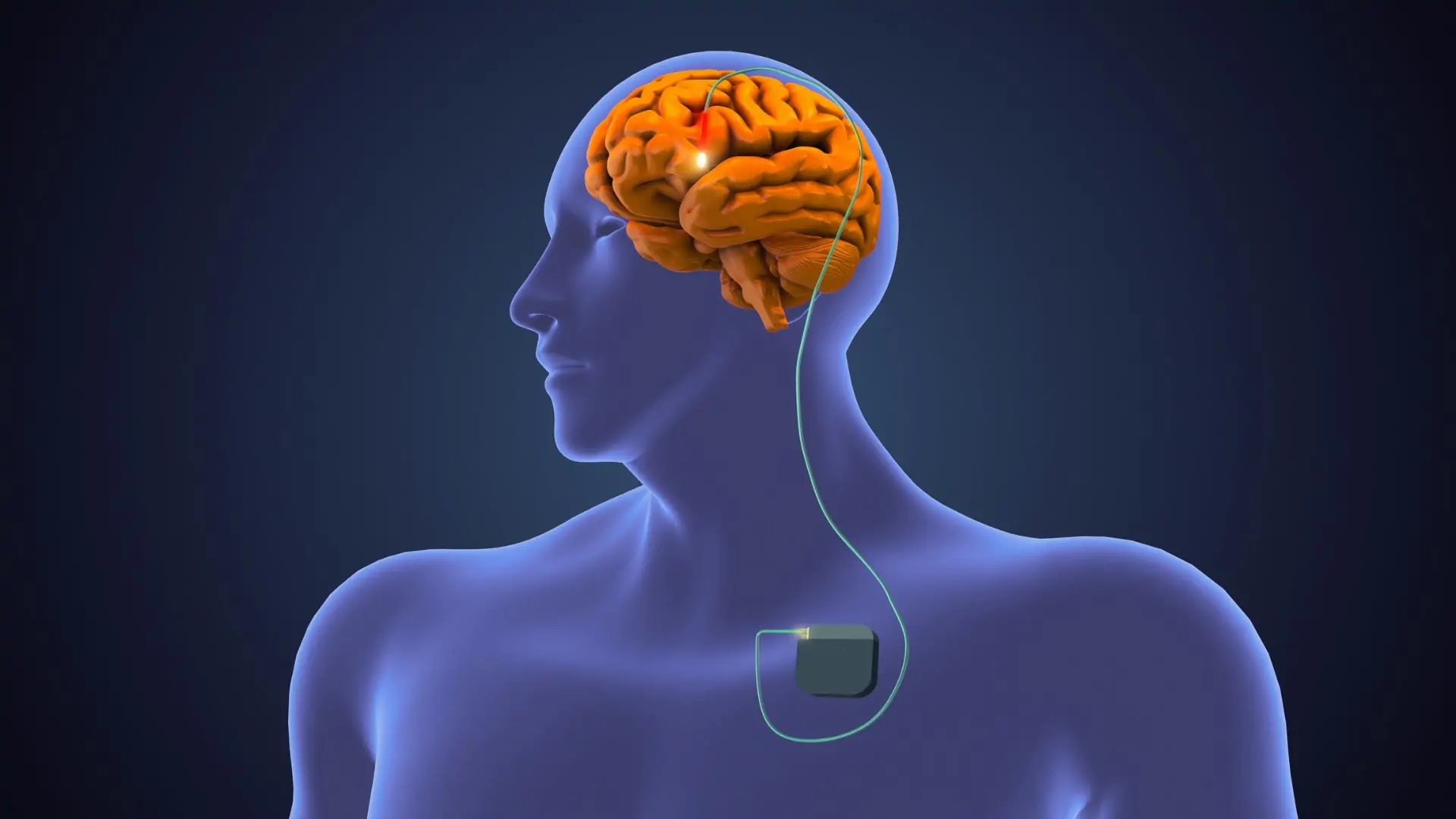
Parkinson Surgery in Noida
ParkinsonÔÇÖs Surgery
ParkinsonÔÇÖs disease is a progressive neurological disorder that affects movement, causing tremors, stiffness, and slowed mobility. While medications remain the first line of treatment, some patients eventually stop responding well to drugs. In such cases, ParkinsonÔÇÖs surgery offers new hope for better symptom control and improved quality of life.
When is Surgery Needed in ParkinsonÔÇÖs Disease?
Medications no longer provide consistent relief
Patients experience severe motor fluctuations
Tremors remain uncontrollable with drugs
Side effects of long-term medications become intolerable
Daily life is significantly disrupted by symptoms
Types of ParkinsonÔÇÖs Surgery
Deep Brain Stimulation (DBS)
Electrodes are implanted in targeted brain areas
A small device (neurostimulator) delivers controlled electrical pulses
Helps regulate abnormal brain signals, reducing tremors, stiffness, and dyskinesia
Adjustable and reversible, making it the most common ParkinsonÔÇÖs surgery today
Lesioning Procedures
Involves creating small, precise lesions in brain areas linked to abnormal movement
Includes thalamotomy and pallidotomy
Less common today but may benefit patients not suitable for DBS
Focused Ultrasound Surgery
A non-invasive option that uses high-intensity ultrasound waves
Targets brain tissue without opening the skull
Useful for controlling tremors in selected patients
Benefits of ParkinsonÔÇÖs Surgery
Significant reduction in tremors and stiffness
Improved movement and daily functioning
Decreased need for high medication doses
Better control of motor fluctuations
Enhanced overall quality of life
Risks and Complications
Infection or bleeding
Device-related complications in DBS
Speech, balance, or memory issues
Rare anesthesia complications
However, with advanced surgical techniques and expert care, most patients experience safe outcomes
Recovery After ParkinsonÔÇÖs Surgery
Hospital stay typically lasts a few days
Device programming sessions are needed for DBS
Symptoms may continue to improve gradually over weeks
Regular follow-ups ensure optimal results
Rehabilitation therapies may be recommended for additional support
